GASTROESOPHAGEAL REFLUX DISEASE (GERD)
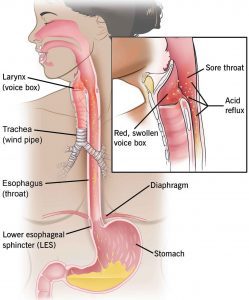
Gastroesophageal reflux disease is a digestive disorder that affects the ring of muscle between your esophagus and your stomach. This ring is called the lower esophageal sphincter (LES). If you have it, you may get hearthburn or acid indigestion. Doctors think that some people may have it because of a condition called hiatal hernia. In most cases, you can ease your GERD symptoms through diet and lifestyle changes. But some people may need medication or surgery.
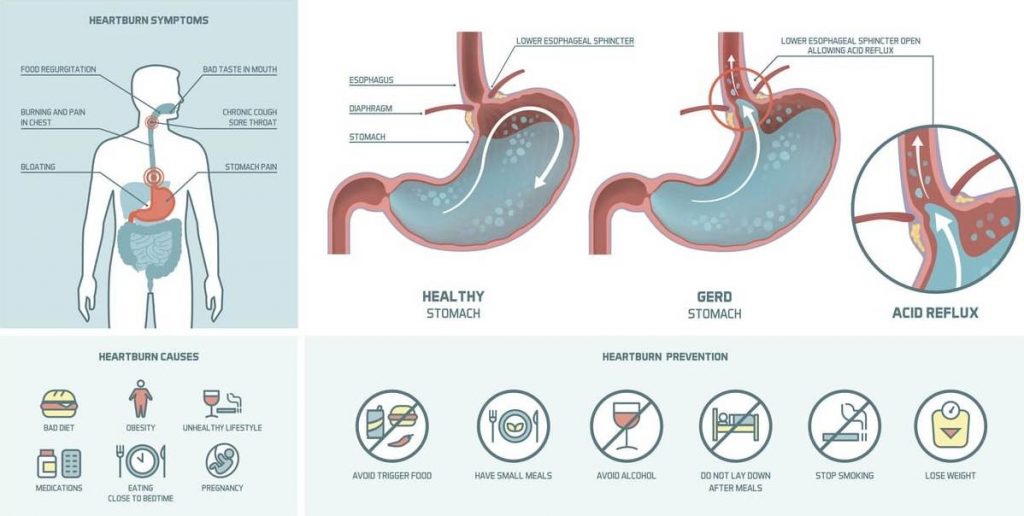
WHAT IS ACID REFLUX AND GERD?
Acid reflux happens when contents from your stomach move up into your esophagus. It’s also called acid regurgitation or gastroesophageal reflux.
If you have symptoms of acid reflux more than twice a week, you might have a condition known as GASTROESOPHAGEAL REFLUX DISEASE (GERD).
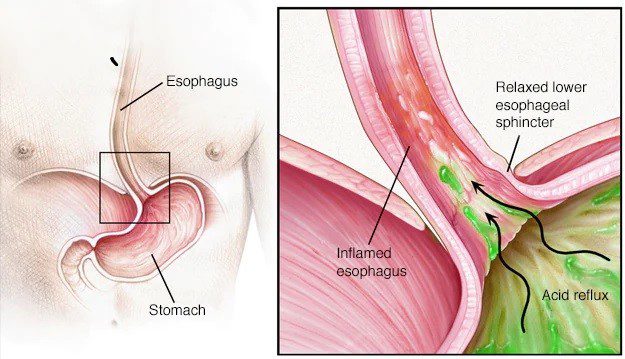
GERD CAUSES:
The term “Gastroesophageal” refers to the stomach and esophagus. Reflux means to flo back or return. Gastroesophageal refflux is when what’s in your stomach backs up into your esophagus. In normal digestion, your LES (opens to allow food into your stomach. Then it closes to stop food and acidic stomach juices from flowing back into your esophagus.
RISK FACTORS FOR GERD:

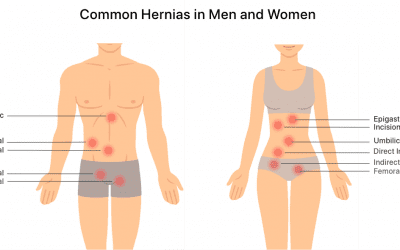
Some doctors believe that a hiatal hernia may weaken the LES and raise your chances of gastroesophageal reflux. Hiatal hernia happens when the upper part of your stomach move up into the chest through a small opening in your diaphragm (Diaphragmatic hiatus).
Several other things can make it more likely that you will have GERD:
- Being overweight or Obese
- Pregnancy
- Delayed emptying of the stomach (Gastroparesis)
- Diseases of connective tissue such as rheumatoid arthritis, scleroderma or lupus
Diet and lifestyle choices may make acid reflux worse if you already have it:
- Smoking
- Certain foods and drinks, including chocolate and fatty or fried foods, coffee and alcohol
- Large meals
- Eating too soon before bed
- Certain medications, including aspirin
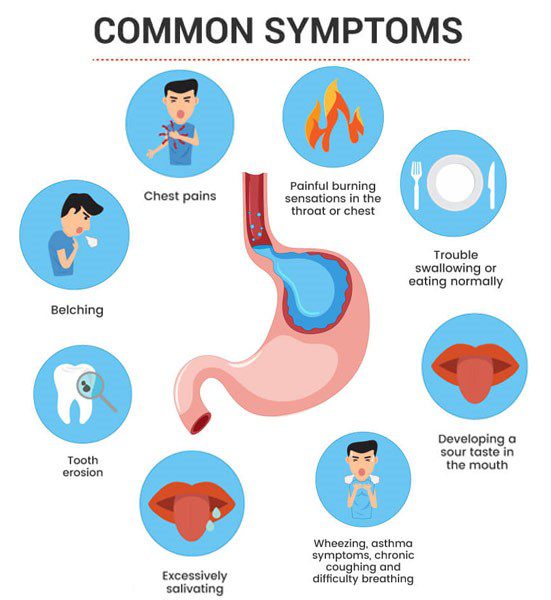
GERD SYMPTOMS:
The most common symptom of GERD is Heartburn (acid indigestion). It usually feels like a burning chest pain that starts behind your breastbone and move upward to your neck and throat. Many people say it feels like food is coming back into the mouth, leaving an acid or bitter taste.
The burning, pressure, or pain of heartburn can last as long as 2 hours. It’s often worse after eating lying down or bending over can also result in heartburn. Many people feel better if they stand upright or take an antacid that clears acid out of the esophagus.
Besides pain, you may also have:
- Nausea
- Bad breath
- Trouble breathing
- A hard time swallowing
- Vomiting
- Wearing a way of tooth enamel
- A lump in your throat
If you have acid reflux at night,You may also have:
- A lingering cough
- Laryngitis
- Asthma that comes on suddenly or gets worse
- Sleep problems

GERD TREATMENT AND HOME REMEDIES:
GERD treatment aims to cut down on the amount of reflux or lessen damage to the lining of the esophagus from refluxed materials.
Doctor may recommend over-the counter or prescription medications to treat your symptoms.
- ANTACIDS:These drugs can help neutralize acid in the esophagus and stomach and stop heartburn. Many people find that nonprescription antacids provide temporary or partial relief. An antacid combined with a foaming agent helps some people.
- H2 BLOCKERS:For chronic reflux and heartburn, doctor may recommend medications to reduce acid in the stomach. These medicines include H2 blockers, which help block acid secretion in the stomach.
- PROTON PUMP INHIBITORS (PPIs): Also known as acid pumps, these drugs block a protein needed to make stomach acid.
- PROKINETICS: In rare cases, these drugs help your stomach empty faster so you don’t have as much acid left behind. They may also help with symptoms like bloating, nausea, and vomiting. But they can also have serious side effects. Many people can’t take them, and those who can should do so only for a limited time.
DIET AND LIFESTYLE CHANGE:
There are several changes that doctors suggest you make in your life style to help lessen your symptoms of GERD:
- AVOD FOODS AND BEVERAGES TRIGGERS:

Stay away from food that can relax the LES, including Chocolate, peppermint, fatty foods, caffeine, and alcoholic beverages. You should also avoid foods and beverages that can irritate a damaged esophageal lining if they cause symptoms, such as citrus fruits and juices, tomato products, and pepper.
- EAT SMALLER SERVINGS:Eating smaller portions at mealtime may also help control symptoms. Also, eating meals at least 2 to 3 hours before bedtime lets the acid in your stomach to down and your stomach partially empty.
- EAT SLOWLY:Take your time at every meal.
- CHEW YOUR FOOD THOROUGHLY:It may help you remember to do this if you set your fork down after you take a bite. Pick it up again only when you have completely chewed and swallowed that bite.
- STOP SMOKING:
Cigarette smoking weakens the LES. Stopping smoking is important to reduce GERD symptoms.
- ELEVATE YOU HEAD:Raising the head of your bed on 6-inch blocks or sleeping on a specially designed wedge lets gravity lessen the reflux of stomach contents into your esophagus. Don’t use pillows to prop yourself up. That only put more pressure on the stomach.
- STAY AT A HEALTHY WEIGHT:Being overweight often worsens symptoms. Many overweight people find relief when they lose weight.
- WEAR LOOSE CLOTHES:Clothes that squeeze your waist put pressure on your belly and the lower part of your esophagus.
SEVERE GERD DIAGNOSIS:
If you have severe, lasting esophageal reflux, of if your symptoms don’t get better with treatment, you may need tests for a better diagnosis. Your doctor may use one or more procedures to do this:
- ENDOSCOPY
- UPPER GI SERIES
- ESOPHAGEAL MANOMETRY AND IMPEDANE STUDY
- pH TESTING
SURGERY FOR SEVERE GERD:
In you need regular high dose of PPIs to control your symptoms, have damage to your esophagus even with medication, and a hitatal hernia, you may need surgery for GERD. But you should try all the other treatments you can first.
FUNDOPLICATION:
This is a procedure that raises the pressure in your lower esophagus. The doctor will wind the top of your stomach around the LES. This tightens the muscle and raises pressure in your lower esophagus to stop reflux. They’ll do this either through a laparoscope (small holes throught the belly) or through open surgery.
TRANSORAL INCISIONLESS FUNDOPLICATION (TIF):
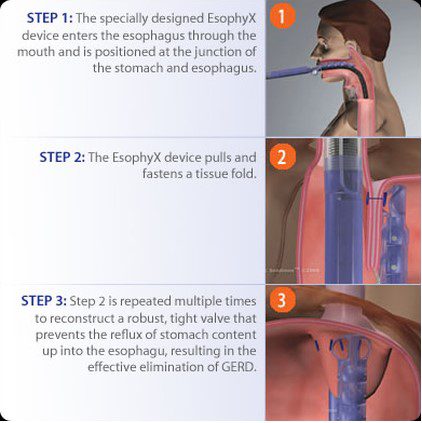
A newer from of this surgery uses an endoscope (a small tube with a camera) to wrap the stomach around the LES with plastic fastener. It’s less invasive than standard fundopication.
STRETTA PROCEDURE:
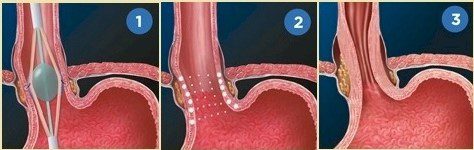
Your doctor puts a small tube down the esophagus that uses low-radiofrequency heat to reshape your LES.
LINX SURGERY:
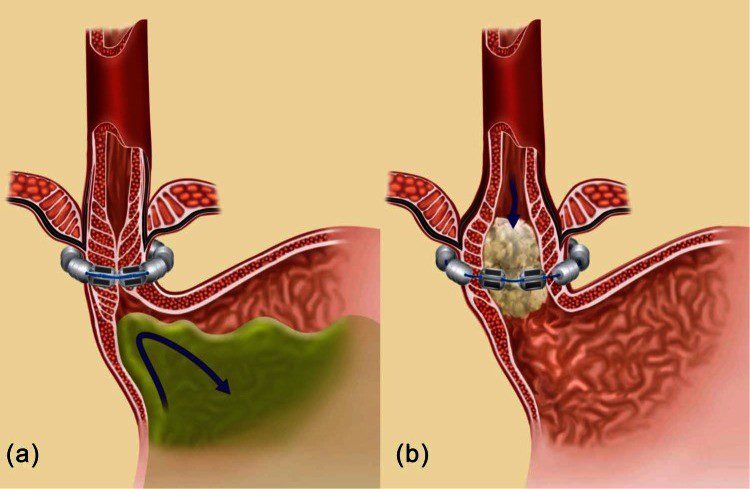
Doctor wraps a band of magnetic titanium beds around the place where your stomach and esophagus meet. The magnetic attraction of the beads keeps it loose enough to let food pass through into the stomach, but tight enough to stop reflux.
GERD COMPLICATIONS:
Sometimes GERD leads to serious complications:
ESOPHAGEAL ULCER:
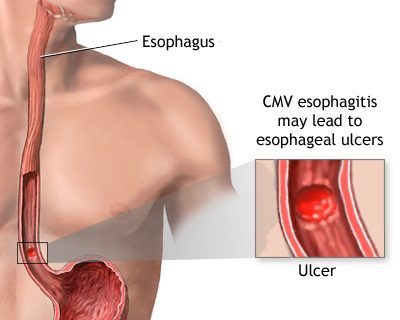
Stomach acid eats away at your esophagus until an open sore forms. These sores are often painful and may bleed. They can make it hard to swallow.
- ESOPHAGEAL STRICTURE:
Stomach acid damages the lower part of your esophagus and causes scar tissue to form. This scar tissue builds up until it narrows the inside of the esophagus and makes it hard to swallow food.
- BARRETT’S ESOPHAGUS:
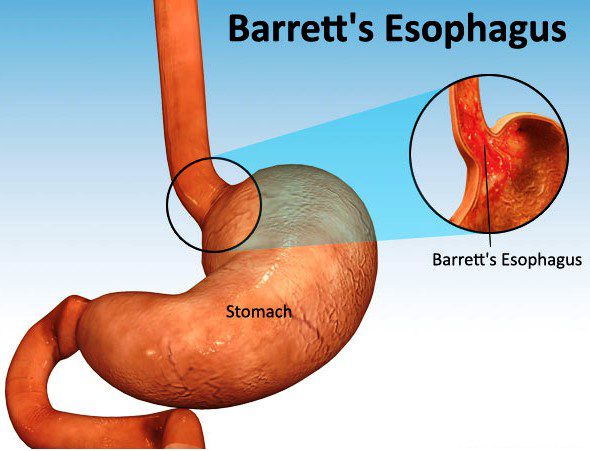
Acid reflux changes the cells in the tissue that lines your esophagus. The linig gets thicker and turns red. This condition is linked to a higher chance of esophageal cancer.
- LUNG PROBLEMS:
If reflux reaches the back of your throat, it can cause irritation and pain. From there, it can get into the Lungs (Aspiration). If this happens, your voice may get hoarse. You could also have postnasal drip, chest congestion, and a lingering cough. If you lungs get inflamed, you can develop asthama, bronchitis, and possibly even pneumonia
VIJAYRAJSINH GOHIL
(G I & LAPAROSCOPIC SURGEON)
(BARIATRIC & METABOLIC SURGEON)
Departments
- Department Of Cardiology
- Neurology
- Nephrology
- Urology
- Spine Surgery
- Orthopaedics/ Trauma
- General Medicine
- General and Laparoscopic Surgery
- Gastrointestinal Surgery
- Bariatric And Diabetes Surgery
- Intensive Care/ Critical Care
- Pulmonology
- Obstetrics and Gynecology
- Oral and maxillofacial surgery
- Dental and Implant surgery
- Neuro Surgery
- Radiology
- Physiotherapy